Menu
Shelley Cohen, RN, MSN, CEN, Triage Champion

The goal of triage is to rapidly identify and sort patients, a critical responsibility for ensuring each patient receives the access and care that aligns with their situation, while appropriately allocating department resources. It's a challenging task for even the most experienced clinical professionals.
While consistency at triage certainly impacts patient outcomes, your triage process can also affect your productivity metrics, liability exposure, patient experience, and nursing attrition rates.
But what if your organization could do more with its triage training process to not only optimize the triage assignment, but also capitalize on the opportunity to positively impact these areas? What if your triage competency and training program could heighten the critical thinking skills of your nursing staff and transform the way triage is performed within your organization?
Before we dive into the structure of an effective competency program, let us confirm an understanding of what we are trying to accomplish.
Competency is the review and documentation of an individual's demonstrated ability to achieve the expectations stated in the job description. It refers to not just the knowledge or understanding of a topic, but the actual ability to apply that knowledge with skill and aptitude for patients.
Several organizations provide guidance on triage nursing competency and the frequency with which it should be evaluated:
American Nurses Association
The ANA states that the public has the right to expect that nurses continue to demonstrate professional competence throughout their careers. Additionally, the process nurses go through should have meaning, promote critical thinking and learning, and be engaging for staff.
Emergency Nurses Association
Years of experience in emergency nursing are not a proxy for initial or continued emergency department triage competency assessment. Triage competency assessment should not be a one-time event, but rather a fluid, dynamic process with periodic assessment of all nurses who practice this high-risk skill.
The Joint Commission
Competency should be validated at least once every three years. The hospital is charged with defining the competencies it requires as well as the methods by which they are assessed. Assessment should be performed by a suitable person upon hire and repeated every three years, or more frequently as required by policy or law/regulation.
DNV GL Healthcare USA
Hospitals must continually evaluate the performance and competency of staff. The process must include use of indicators that will objectively measure the ability of staff to perform all duties outlined in the job description. The policy/practice the hospital uses to validate staff occurs within a specific time frame, no less than once per calendar year.
Previous Step
Next Step

Previous Step
Next Step
Previous Step
Next Step

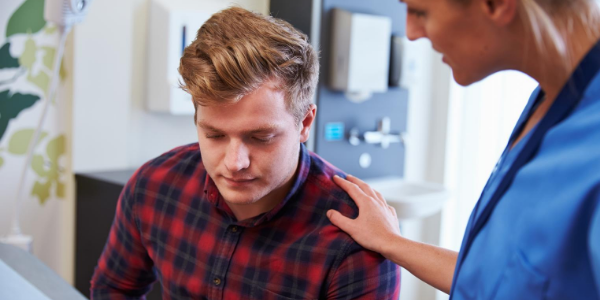
The first step in ensuring competency is selecting the right candidates to train for the role of the triage nurse. Each organization should create its list of requirements a nurse must meet before enrolling in a triage training program to ensure the highest quality patient care.
Consider the following as you create your list:
"The triage process is best carried out by registered nurses and nurse practitioners with emergency nursing expertise who have completed a triage-specific educational program." ENA Position Statement on Triage Qualifications & Competency 2017

Once a nurse has been selected for triage training, there is a baseline level of competency that should be met, whether the nurse is a novice or an experienced new hire.
As you develop what triage competency means in your organization, consider the following:
Before triaging independently, nurses need to have a concrete understanding of the following baseline triage concepts:
Once your baseline competencies are defined, what methods will you use to help new hires acquire this initial competency? At a minimum, a new hire should expect:
Previous Step
Next Step

Define a formal education program that each new hire must successfully complete as part of their training program. An example of a best practice education program is The Sullivan Group's Triage Fundamentals Program, created by experienced triage trainers, to ensure nurses have a concrete understanding of the core concepts critical to triage success.
If your new hire has prior healthcare experience, you might modify their formal education requirements or timeline. Some organizations offer a test-out option for experienced nurses to bypass certain courses.
You can read more about how to structure your triage education program here.
Previous Step
Next Step

Be mindful that each nurse has a unique learning style. Your program should incorporate a variety of teaching and assessment methods so each nurse has the opportunity to grasp concepts and be successful.
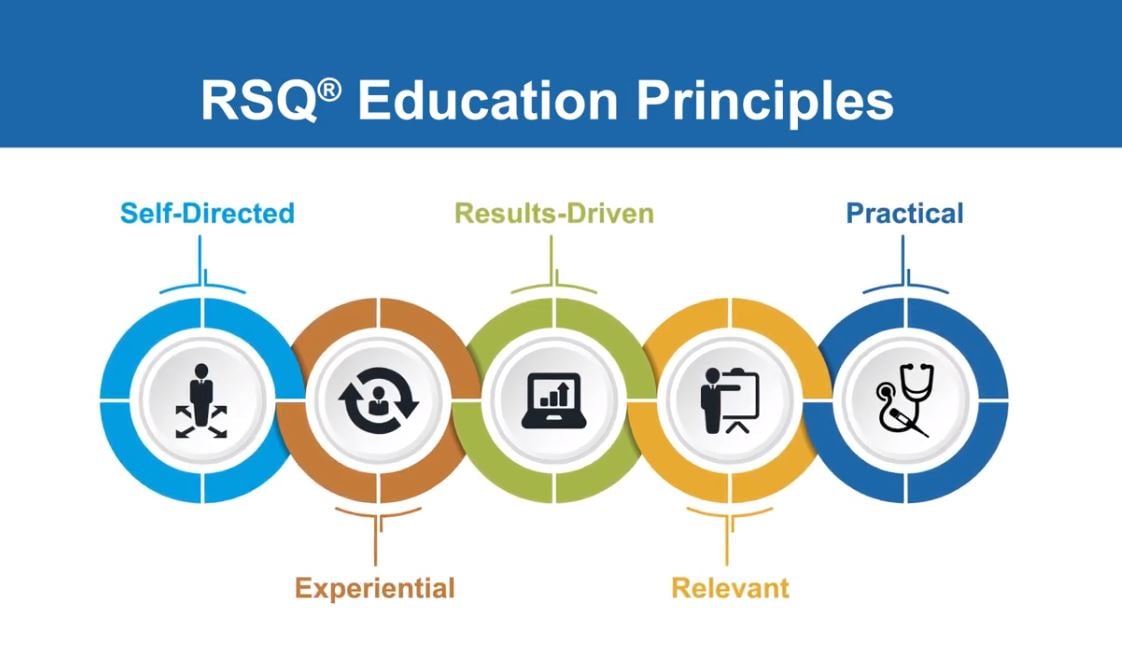
As a model, The Sullivan Group's education programs are built upon our RSQ® Education Principles consisting of five core pillars of educational excellence for adult learners.
Learn more by watching this video outlining our pillars of educational excellence.
Previous Step
Next Step
The next critical step is to develop a system and schedule to verify those triage competencies.
Before creating the schedule itself, let us review a variety of competency validation methods. Each has its strengths and weaknesses. It is important to create a program that incorporates multiple methods to capitalize on the nurse's individual learning and performance style.

Case review scenarios allow nurses to put themselves in situations they might not yet have experienced firsthand. However, a study in The Scandinavian Journal of Trauma, Resuscitation, and Emergency Medicine (Jordi) found that nurses overestimate the accuracy of their acuity level assignment; therefore, standard written case scenarios may not be the optimum method to rate nurse triage skills.
The study aimed to determine accuracy, inter-rater reliability, and subjective confidence of 69 triage nurses at four hospitals to determine ESI acuity level. Nurses applied the ESI scale to 30 teaching case scenarios. Collectively the group only scored 59.6% of cases correctly, but 78% of the nurses felt confident in their ability to apply ESI.
This overconfidence underscores the need to diversify your competency validation strategy.
While the Emergency Nurses Association (ENA) has historically recommended ongoing competency validation to ensure safe practice in the ED, the organization updated its Triage Qualifications and Competency Position Statement in 2017 to place greater emphasis on the use of retrospective chart review as a means to ensure accurate clinical decision-making in triage.
In addition to the ENA recommendation, there are seven additional reasons retrospective chart review is an effective a part of a triage competency validation process:
Retrospective chart review can be performed by self-assessment or peer review. Reviews should answer questions such as:
While your initial formalized triage training and onboarding process might span six to twelve months, the evaluation of triage competency is ongoing. Not only is ongoing competency validation a regulatory requirement, but it also promotes consistency in triage regardless of who is performing the task.
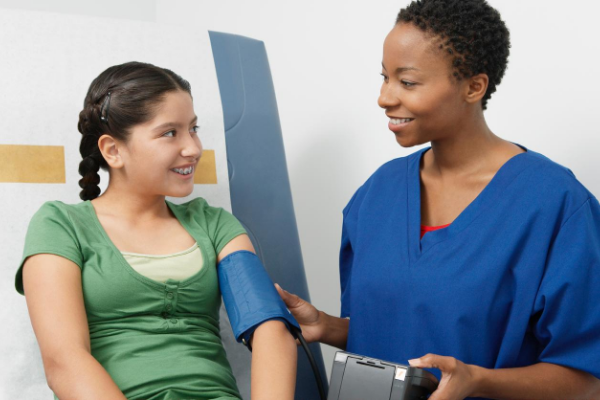
There are always new things to learn, like updated standards or incorporating a new documentation standard/requirement. Additionally, there are constant opportunities for improvement, especially related to the sorting of high-risk patients and seconds-to-minutes emergencies that have mandated order sets.
Consider these questions as you strive to optimize triage competency:
You might also rotate through a list of frequent chief complaints or diagnoses as part of your ongoing competency process.
According to 2017 data from the Centers for Disease Control (CDC), the principal reasons for emergency department visits nationally include:
Available by request via your IT or billing department, a report of frequent diagnosis codes by month or year might also prove valuable in uncovering areas of focus.
Chart reviews focused on any one of these highlighted areas can uncover common pitfalls related to frequent complaints or high-risk diagnoses, providing an opportunity for practice improvement.
Based on these best practice concepts, below is an outline of how an organization might define its competency requirements, activities, and schedule.
While this can provide a foundation for your program, keep in mind that your triage competency process should be dynamic and responsive to changes in the environment.
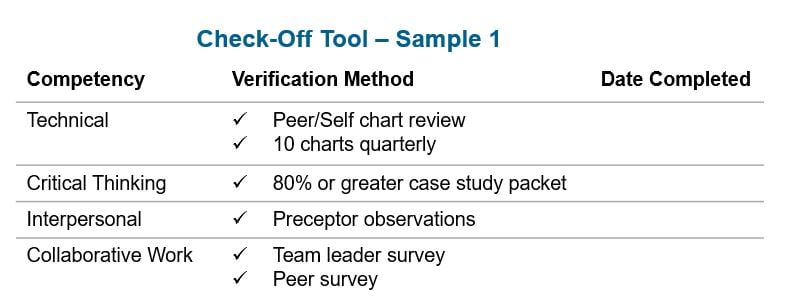
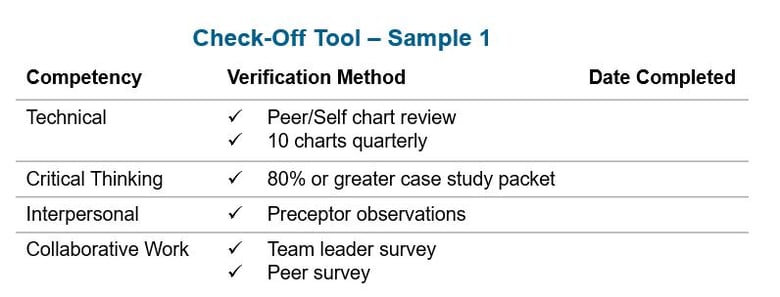



Once you have solidified the structure of your triage competency program, it's critical to share it with your staff so they know what to expect. Define in writing what happens if someone fails to complete the triage competency requirement for any reason or if their performance doesn't meet standards.
Failure to meet your standards might result in remediation strategies, such as increasing retrospective chart review requirements.
It is critical to also consider whether someone needs to be reassigned in the interest of patient safety.

Engaging staff in the development and modification of your triage competency process can increase program buy-in and compliance. Once you have developed your program, share it with staff and educate them on the reasoning behind the methods included. Ask them for feedback on how to improve the process.
For example, some organizations survey staff to ask for feedback on modifications to annual triage competencies, including preferences such as more peer reviews, fewer chart reviews, multiple-choice exams, more case scenario packets, etc.
Inevitably, you'll encounter obstacles to implementing triage best practice and competency improvement, especially from those who prioritize tasks over critical thinking and vital signs over red flags for demise; thus the importance of ongoing training to address these gaps in practice.
Another challenge clinical educators and nursing leaders may face is the lack of staff engagement in the training process. Some organizations combat this hurdle by offering paid time outside of shifts to complete training and competency requirements. Providing resources like computer labs and internet access also demonstrate the importance of their continuing education to your organization and their role within it.
Designed for clinical leadership and hospital administrators, this free resource outlines how to implement a sustainable triage training program.
After reviewing this playbook, you will have a greater appreciation for:

Nurses stay in roles where they feel valued, respected, and appreciated. Recent studies of nursing turnover cite cost ranges from $22,000 to $64,000 per nurse. Investing in the continuing education and practice improvement of your nurses shows your commitment to their extended tenure with your organization.
Providing the tools your staff needs to be successful also increases job satisfaction and ensures each nurse feels competent. This starts with the foundational training we've outlined above. Additionally, it prepares them to be successful in difficult situations because it will not be the first time they will have encountered the issue, whether related to an acutely agitated patient, an intoxicated patient, or a behavioral health patient.
A recent CRICO study demonstrated the increased frequency with which nursing is cited as the primary responsible party in malpractice suits claiming a failure to follow a policy or protocol.
Protect your nursing staff from medical-legal issues by ensuring they have a working knowledge of the regulations that open them to malpractice. Critical concepts include EMTALA, boarding of behavioral health patients, and abuse detection for vulnerable populations such as child abuse, elder abuse, human trafficking, and intimate partner violence.
Requests for new programs meet increasing scrutiny due to the budget constraints many organizations face. Investments made in training programs need to result in measurable changes.
We encourage organizations to look to the following departments for potential funding of an updated triage training program:
Learn more about making the business case for a new program with each of these departments in this Triage Playbook.
If budget constraints are an issue, it is understandable why some organizations suggest you build your triage training solution internally.
However, this option can be less desirable when you factor in the costs of maintaining current content, the risk of not achieving results, and the turnover within the clinical education role. There is also benefit to using a training system built by experienced triage trainers and optimized through the feedback of its clients, including some of the largest health systems in the country.
While education provides foundational knowledge, it doesn't necessarily imply that a nurse can apply that knowledge in the actual practice setting. Beyond training, you need a mechanism to measure competence – the application of ability, skill, and aptitude with patients. For this reason, many regulatory bodies recommend a competency validation process that includes education to address knowledge gaps and validation methods, such as those discussed here, to confirm that knowledge can be successfully applied in practice.
